| « Youth In Play: Ameya Pawar and the People | Pilsen Residents Lead on Lead » |
Health Care Thu Apr 14 2011
Nurses See Extra Burden in South Side Emergency Rooms
This article was submitted by freelance journalist Samantha Winslow.
![nurserally1[1].JPG](http://gapersblock.com/mechanics/assets_c/2011/04/nurserally1[1]-thumb-300x199-6745.jpg) Reasheal Lehmann joined the line of people on East 59th Street in front of the University of Chicago Medical Center. An emergency room nurse at the hospital, Lehmann wore bright red scrubs emblazoned with her union's logo, National Nurses United; others wore raincoats and parkas, trying to stay warm on an unusually cold March evening. As the sun went down, the University buildings glowed with yellow light like a cathedral. More nurses ended their shifts and they also came outside.
Reasheal Lehmann joined the line of people on East 59th Street in front of the University of Chicago Medical Center. An emergency room nurse at the hospital, Lehmann wore bright red scrubs emblazoned with her union's logo, National Nurses United; others wore raincoats and parkas, trying to stay warm on an unusually cold March evening. As the sun went down, the University buildings glowed with yellow light like a cathedral. More nurses ended their shifts and they also came outside.
Staff nurses at the medical center, which is affiliated with one of the nation's most prestigious universities, are in union negotiations with the hospital and one of their key issues is staffing levels. The candlelight vigil was intended to bring public attention to what they say is a crisis in emergency room care on the city's South Side.
"It's already a tough situation to begin with," Lehmann says, "We are seeing not only a bigger volume of patients but a higher acuity of patients." She says patients are coming in often with multiple illnesses, and a higher severity of illness. The risks of overcrowded emergency rooms are not having enough nurses and staff to assess and treat patients in a timely manner.
Their concern is if there aren't enough nurses in an emergency room to handle a high volume of very sick patients, people could slip through the cracks. Last year, UCMC paid a $50,000 fine after a 78-year-old died after waiting 4 hours in the emergency room.
Many people say the status of South Side emergency departments has been grim for a long time, with seven area hospitals closing in the past 25 years. But for Lehmann, the situation in the emergency room is more critical now than ever. Provident, a county-run hospital less than two miles away, has downsized over the years and in February, closed its doors to admissions by ambulance.
"Since Provident closed, the situation has been exacerbated," Lehmann says.
Even though a mere 10 percent of their ER patients arrived by ambulance, Provident's decision still reflects the shrinking number of South Side hospitals accepting ambulances, and the general shortage of access of emergency services for the community.
Lehmann says that because UCMC closed general medicine units over a year ago, fewer beds are available in the hospital for patients once they are stabilized in the ER.
That means patients must stay for as long as 48 hours instead of being admitted to the hospital and getting a room. They are in a no man's land; they wait on a cot, without a phone, TV, pillows, curtains. Those patients take up much-needed space in the ER for new patients to be seen. Critics see both making both patients wait in ER beds and bypassing ambulances, as prioritizing specialty patients over emergency room patients who often are not on private insurance. ER doctors publicly criticized the move to reduce beds for ER cases in February 2009, including two doctors resigning from their administrative posts at the hospital.
Lehmann believes that the status quo doesn't have to be this way. "It's stressful," she says, "How do you tell these patients the reality of how they are being treated by the hospital?"
![nurserally2[1].JPG](http://gapersblock.com/mechanics/assets_c/2011/04/nurserally2[1]-thumb-300x199-6748.jpg) She says that by allowing nurses' input that would appropriately increase personnel for departments like the ER, it will alleviate the long waits for patients, especially if the ratios are based on acuity or severity of the patients' illnesses. In specialty departments, there can be as few as two nurses per patient. Lehmann and fellow nurses want to have input on creating a lower nurse-to-patient ratio for their department and throughout the hospital that takes into account how serious a given patient's condition is. This is one of the contract priorities for the nurses. "It's a huge thing that we are bargaining over," she says.
She says that by allowing nurses' input that would appropriately increase personnel for departments like the ER, it will alleviate the long waits for patients, especially if the ratios are based on acuity or severity of the patients' illnesses. In specialty departments, there can be as few as two nurses per patient. Lehmann and fellow nurses want to have input on creating a lower nurse-to-patient ratio for their department and throughout the hospital that takes into account how serious a given patient's condition is. This is one of the contract priorities for the nurses. "It's a huge thing that we are bargaining over," she says.
Other area hospitals share in long wait times for ER patients, particularly the county hospital less than two miles from UCMC. Outside of Provident Hospital, the red emergency sign is faded and chipping away, and many of its halls are quiet. Provident has gradually closed departments, including Labor and Delivery and Telemetry, as it downsized.
The shut-down ICU looks like it is frozen in time. The gurneys are still there, and pictures of staff are still up on the walls, but no patients are being treated.
Imelda Allen, who has been a nurse at Provident since 1976, says not taking ambulances is a reprieve for the hospital, but not a solution for the patients who still need treatment. Wait times in the walk-in emergency room are still long, and they have far less beds than UCMC's ER.
As part of the Cook County system, Provident sees patients with the least options, often the uninsured. Allen says people can wait from 8 to 19 hours once they are in a stabilized and in an ER beds. And with cutbacks, staffing is short, which is hard on the nurses and hospital workers. "The stress level is very high," she says. "We have patients coming from all levels."
Since the hospital has limited services, many of the patients are sent to Stroger Hospital, the main county hospital on the Near West Side.
Allen points out the general crisis in emergency services that led to Provident closing doors to ambulances. "University of Chicago always on bypass, Saint Bernard is on bypass, Mercy is always full," she said referring to the remaining South Side hospitals.
A Chicago Sun Times investigation found that in 2010, UCMC spent 1,764 hours on bypass, amounting to 22 percent of time. Now it is estimated they are on bypass often as one-third of the time.
"They shouldn't turn down people," Allen says.
The burden on emergency rooms comes partly from people not using primary care services or preventive care. And on the South Side, it's understandable. The area that surrounds the University of Chicago is often called a healthcare desert. The wait times at the Provident outpatient services are long. Some doctors are booked through the end of the year.
"You should not sit in the middle of a community that is so in need," Deborah Taylor says about the University of Chicago. She came to the candlelight vigil to support the nurses, and speak out about the lack of health care options on the South Side.
Representatives from University of Chicago point out that the emergency department's high volume is not a new situation, and that in general, ERs are overcrowded--particularly in urban areas--around the country.
"It's not just the University of Chicago, it's not just the South Side," says Dr. Robert Mulliken, a senior faculty member at the University who used to head the Emergency Department.
Mulliken says the when the hospital makes the decision to go on bypass and not take ambulances, it is for a legitimate reasons--they don't have room to spare. He stressed that urban area emergency rooms are busy places by the nature of the service they provide.
Living in the area, and being on disability, Taylor goes to the University of Chicago's dialysis clinic, along with four other UCMC clinics where she gets her healthcare needs met.
She says the Urban Health Initiative, which was led by First Lady Michelle Obama during her time working at the University, is an example of the Hospital's shift in priorities.
The Initiative's mission is to redirect low-income South Side patients to community clinics, rather than having them rely on emergency rooms for health care. The Chicago Tribune reported in 2010 that more than 3,000 new patient visits and a 40 percent increase over five years, in the network of community clinics on the South Side. These visits are credited to UCMC's education and referral process, showing that clinic visits are better for patient health, and less costly than ER visits.
But Deborah Taylor questions why the UCMC is sending people away from their own medical center for health care,"We could fall into their door," Taylor says, "and they don't want to see us,"
But in 2009, the American College of Emergency Physicians criticized UCMC's emergency room practices, notably its long waits and diverting of patients to other hospitals saying that the Urban Health Initiative comes dangerously close to patient dumping, a violation of federal law.
Taylor criticizes the clinics for being rundown and substandard. "Some of the clinics that [UCMC] used for their health initiative," Taylor says, "Are the clinics I wanted to avoid." She says the hospital doesn't want to treat patients without private insurance. An example of further cuts in services is a women's clinic that UCMC closed in 2009 as part of cost cutting measures. The clinic director's said that the closure would increase health access disparities among the thousands of women who were patients there each year.
Taylor insists on being treated at UCMC because the hospital is the best option in the area, and because she likes her doctors and has built a relationship with them over the years. "Because I'm black or because I'm poor, I'm not entitled to good care?"
She is an activist with South Side Organizing for Power, who protested around the need of a South Side adult trauma center, another issue the university has not addressed since they closed theirs in 1988. The community organization's mission centers on the story of Damian Turner, a teenager who was diverted to Northwestern Memorial Hospital to treat a fatal gunshot wound in August 2010, after being shot four blocks from UCMC. Their have actions by the hospital frequently, and came to the nurses vigil in support. They are planning another vigil outside UCMC April 21st, to continue pressure to hospital and bring attention to the issue.
Now Taylor worries that if she needs an ambulance because of her health problems, she might be diverted to a hospital further away on the West Side or the Far South Side. She worries that even though UCMC is the closest hospital to her, the extra time in ambulance taking her across town could put her health in jeopardy.
One of the pressure points that the nurse union and community groups use is UCMC's tax-exempt status. The private not-for-profit hospital ranked in the top three metro area hospitals according to U.S. News and World Report,
and is in the process of adding a $700 million medical pavilion to their current location in Hyde Park. Both hospital employees and concerned community members want to show that the University should give back more to the community for the money they keep in tax breaks.
Mulliken emphasizes the challenges of being the only university hospital in the area, and says the hospital treats a disproportionate share of Medicaid and Medicare patients compared to similar area hospitals. A 2009 report by the Center for Tax Accountability calculated the amount of charity care--defined as reduced or no-cost care for low-income patients--required by law of non-profit hospitals, and compared that figure with their tax exemptions. Their findings showed that UCMC spent $10 million on charity care, compared with $50 million they saved with the tax breaks.
Margie Schaps of the Health and Medicine Policy Research Group points out that the University of Chicago could do more in charity care, but that only addresses part of problem: the of lack of options for the uninsured and underinsured. As executive director of a policy and advocacy organization that works to address health care access and affordability issues, Schaps sees both sides of the debate. "Hospitals are businesses. They are trying to balance their needs with the community."
She says these problems will continue "As long as we don't put the right amount of money into the public health system."
The issues of charity care are being discussed at the state level. The Hospital Fair Care Act, which was introduced earlier this year to the Illinois General Assembly, would require 3.5% of a tax-exempt hospital's revenue to go to charity care, which is far more than what UCMC currently spends on such cases.
All of the sides of this debate can agree that the bigger challenge is increasing healthcare options for residents on the South Side. When national healthcare reform is implemented in Illinois, Schaps estimates half a million more people will be insured in the Chicago area, and that may help people access primary healthcare, and have insurance for emergencies. She tempered that promising news with concern that the public health system will still be strained.
A few weeks after the vigil, with little progress in union negotiations with the hospital, Reasheal Lehmann ends her shift in the emergency room after seeing patients who had to wait 16 hours for treatment. Her frustration comes through in the conversation. "It's always going to be a busy ER," she says. "That's not the issue."
To Lehmann, the problem can be solved if UCMC adds more nursing staff and opens more general medicine beds in the hospital, letting those who come in through the ER be treated sooner. She makes her priorities clear. "As nurses, we don't deal with insurance. I'm there regardless," she says, "To me, once you walk through those doors, you are a patient."
Samantha Winslow is a free lance writer based in Chicago who recently graduated from Medill Journalism School. Before her career change into journalism, she was union organizer in California. She writes about health care, housing, labor, and education.
This feature is supported in part by a Community News Matters grant from The Chicago Community Trust and the John S. and James L. Knight Foundation. More information here.

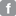

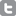

![nurserally3[1].JPG](http://gapersblock.com/mechanics/assets_c/2011/04/nurserally3[1]-thumb-350x233-6751.jpg)






Anne Scheetz / April 16, 2011 9:03 PM
I am a member of Physicians for a National Health Program and the Illinois Single-Payer Coalition, and I attended the candlelight vigil at U of C. One of the speakers was Dr. Philip Verhoef, who pointed out that under a single-payer health care system all patients would be insured under the national health plan, and hospitals would be compensated for the care of all patients. Single-payer health care is a win-win-win for patients, communities, and hospitals. We don't need to put more money into health care. If we stop supporting the wasteful and useless private health insurance industry and instead use that money for health care, we will be able to take care of everybody without spending a penny more.